The immune system is the body’s defense against harmful agents. It provides immunity.
Immunity is the ability of the body to resist all forms of organisms and their toxins, which tend to damage the body’s cells and tissues.
This resistance to particular infectious microbes or toxins is mediated by the specific action of antibodies or sensitized white blood cells released by the immune system.
Components of the immune system:
The immune system is comprised of
- Organ-based
- Cellular-based
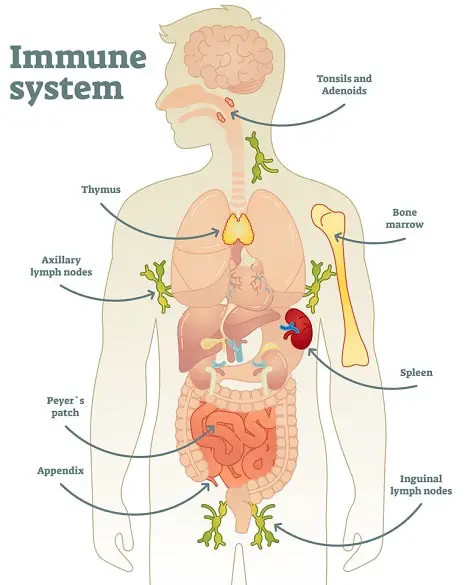
The organs of the immune system are distributed in different places in the body.
These are differentiated as
Primary lymphoid organs:
- Thymus
- Bone marrow
Secondary lymphoid organs:
- lymph nodes,
- Spleen, and
- mucosa-associated lymphoid tissue (MALT)
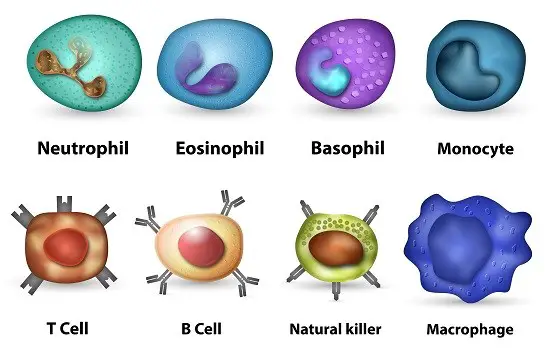
The cellular-based immune system comprises immune cells like monocytes, macrophages, lymphocytes, basophils, neutrophils, and eosinophils.
- The immune organs help in either the formation of immune cells or in trapping pathogens or exposing them to immune cells.
- These immune cells perform the actual function of defense either by producing antibodies or by eating the pathogens through phagocytosis.
Types of immunity
This immunity is of two types as
- Natural or innate immunity
- Acquired or adaptive immunity
Natural immunity is resistance to microbes, toxins, and other infections.
This is not specifically directed against a particular organism or strain of microbes. This is also a part of physiology.
This includes
a) Phagocytosis of microbes like protozoa, bacteria, fungi, etc., by the white blood cells.
b) Acidic and enzymatic destruction of foreign microbes in the digestive tract.
c) Prevention of invasion through the skin.
d) Foreign organisms and cells in the blood are destroyed due to the action of lysozymes, polypeptides, and natural killer cells.
Thus, natural immunity is the nonspecific defense that keeps the body free from pathogenic microorganisms.
Acquired immunity
- This form of immunity develops due to the body’s exposure to external infectious microbes and toxins.
- It is powerful and extremely specific against individual microbes like pathogenic bacteria, protozoa, viruses, etc.
- Here, the body will develop specific counter-effects in the form of antibodies and killer cells, which can destroy the foreign agent if exposed again.
- This phenomenon of agent-specific immunity is used in mass vaccination to prevent future infectious attacks.
This acquired immunity works by two mechanisms
a) Humoral immunity or B-cell immunity,
b) Cell-mediated immunity or T-cell immunity.
- Humoral immunity works by the release of antigens or immunoglobulins by B-cells.
- Cell-mediated immunity works by direct destruction of foreign cells.
- These antibodies bind to the pathogenic microbes and neutralize them.
- This occurs due to the cells, like the macrophages, neutrophils, and natural killer cells
Mechanism of immunity
- In short, the body recognizes the foreign cells through their surface antigens.
- As a response, it produces antibodies and phagocytic cells to destroy those foreign cells.
- For a substance to be antigenic, it should have a molecular weight of 8000 or more.
- An antigen is mostly a protein or a large polysaccharide molecule. When it is introduced into the blood, it stimulates antibody production.
An antibody is, again, a protein substance that binds to an antigen; there are five classes: Immunoglobulin G (IgG), IgA, IgM, IgE, and IgD.
| Immunoglobulin | Its Character | Functions and Effects |
|---|---|---|
| IgA | This antibody activates an inflammatory response. They are found in profuse numbers during allergies. | Prevents the antigens from passing through the epithelial membranes and deep tissues. |
| IgD | It is present on the surface of B-lymphocytes | They bind to antigens and activate the B-cells to release antibodies. |
| IgE | This antibody is present in the cell membranes of mast cells, basophils, and so on. | It attacks a wide range of pathogens and even crosses the placenta to protect the fetus in the womb |
| IgG | This is the largest and most common antibody. | It activates the complement system. |
| IgM | They are found in large numbers during primary acquired immunity. | This is the largest and most commonly found antibody. |
Antigen recognition
- They possess cell surface receptors for several extracellular molecules, including cytokines, selectins, integrins, and FC (constant fragment of an antibody.
- These receptors recognize the organism and initiate intracellular mechanisms in macrophages.
- The antigen becomes recognizable and can also be coated by antibodies or complement. This process is termed opsonization.
Phagocytosis:
- Phagocytosis is the cells’ engulfment of solid particulate material (cell-eating).
- The cells performing this function are called phagocytes.
There are two main types of phagocytic cells.
- Polymorphonuclear neutrophils (pens): These appear early in the acute inflammatory response, sometimes called macrophages.
- Circulating monocytes and fixed tissue mononuclear Phagocytes are commonly called macrophages.
Secretory function: macrophages secrete important biomolecule substances as follows.
- Cytokines and prostaglandins are chemical mediators that activate other leukocytes.
- Secretory proteins involved in wound healing, eg, Collagenase, elastase, fibroblast growth factor, and angiogenesis factor.
- Acute phase reactants, e.g., fibronectin, microglobulin.
Antigen presentation:
- If the macrophages cannot lyse an antigen or an organism, the next best course they adopt is to act as antigen-presenting cells for presenting to immunocompetent T cells (subtype CD4+ OR CD8+ cells) or B cells.
Basophils and mast cells:
- Basophils are a type of circulating granulocyte (0-1%),
- While the mast cells are their counterpart seen in tissues, especially in connective tissues around blood vessels and submucosal locations.
- Basophils and mast cells have IgE surface receptors; thus, on coming in contact with an antigen binding to IgE (e.g., allergic reaction and parasites), these cells get activated and release granules, i.e., degranulate.
- These granules contain Histamine, platelet-activating factor, heparin, and certain chemical mediators.
- Mast cells and basophils mediate inflammation in allergic reactions and have a role in wound healing.
Neutrophils:
- Polymorphonuclear neutrophils (PMNs) are normally the most numerous circulating leucocytes (40-75%).
- The cytoplasm of the OMNs contains lysosomal granules of three types: primary, secondary, and tertiary.
- The PMNs function similarly to macrophages and are therefore appropriately referred to as macrophages, owing to their role as the first line of defense against an invading foreign organism in the body.
The cells have limited sizes and types of organisms to be engulfed.
Eosinophils:
- Eosinophils also circulate granulocytes(1-6%).
- These cells play a role in allergic reactions and intestinal helminthiasis.
- The granules of Eosinophils contain lysosomal enzymes, peroxidases, and chemical mediators of inflammation (prostaglandins, leukotrienes).
