Bacteria are single-celled microorganisms that are invisible to the naked eye.
They are classified under plants and not animals due to similar resemblances.
However many bacteria infect humans and animals, causing deadly diseases.
They can act as parasites in almost all human body organs.
Further, they quickly spread from one person to another, utilizing water, air, food, insects, sex, etc.
So bacterial identification is a necessary part of disease diagnosis and cure.
Without identifying causative bacteria, it is tough to provide effective treatment with available antibiotics.
Bacterial Identification methods
So we identify them using a microscope, by enhancing their population to a huge bulk, or by biochemical methods.
Hence, in identifying bacteria, we use microscopical, medical, biochemical, & serological methods.
1. Identification by morphology
This method is to determine the individual bacterial physical appearance.
a. Based on size
Here, bacteria are identified based on their physical size, like small size or big ones expressed in microns. For this, bacteria are viewed under a microscope to consider their size. One can apply some stain to the culture and use methods like glass slit or hanging drop method.
In the glass slit method, a layer of bacterial culture is applied, stained, and viewed by a microscope above 40x magnification.
In the hanging drop method, a drop of culture is made to hang between the glass slide and slit and viewed under a microscope. The glass slide has a concave aperture on one side at the center where the glass slit with culture drop is placed over such that drop suspends in the concave aperture. The advantage of the hanging drop method is we can identify motile bacteria.
b. Based on the shape.
The structure of bacteria varies spherical (cocus), bar or stick-like (bacilli), chain-like (strep), and comma-shaped like vibrio-cholera bacteria.
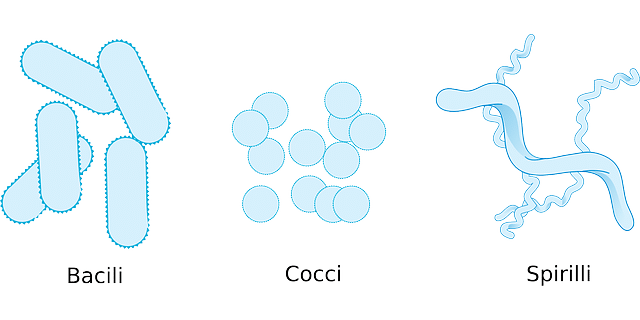
Even the shape of the bacteria colony grown on the nutrition medium also differ for different strain of bacteria.
Hence, under the microscope, the bacterial colony radius and shape can be viewed, and the strain of bacteria can be identified.
c. By extra-cellular characters
Here, some extra-cellular characters are used in the identification of bacteria. Some bacteria have flagella for motion.
So, they can be identified based on the number of flagella and the arrangement of flagella on the bacterial surface.
Ex: Atrichous bacteria have no flagella, Monotrichous have one flagellum, and Polytrichous have many flagella.
Even some bacteria have two flagella, one on each side of the cell.
2. By Culture characteristics
Here, bacteria cultures as a whole are identified.
Since most bacteria grow in colonies and divide fast, they can be easily grown into a culture in suitable nutrition media.
Based on the characteristics of the culture, they can be identified as
- The shape of culture: Circular, irregular, rhizoid, etc.
- Size of culture or colonies in millimeters.
- Type of elevation of culture like effuse, convex, concave, etc.
- Margins of the colony like dentate, rough, smooth, etc.
- The surface of the colony: Smooth, wavy, papillate, etc.
- Color of culture.
3. Based on resistance
Antibiotics are specific to certain bacteria. Hence, few bacteria develop resistance to certain types of antibiotics.
By adding the antibiotics to the culture and measuring the resistance of the microbe to the said antibiotic, the type of bacteria can be identified.
Ex: TB bacteria, i.e., Mycobacterium tuberculosis, is not affected by penicillin but killed by ciprofloxacin.
So, this differentiation can be used to identify a few bacteria.
4. Based on metabolism features
Few bacteria are so specific for metabolic requirements. Based on this specificity, they can be identified.
Ex: Aerobic bacteria require oxygen for survival.
Anaerobic bacteria get killed when exposed to oxygen. Similarly, some require carbon dioxide, blood, or other pigments for metabolism.
5. Through biochemical tests.
This is one of the most widely used methods and more important.
a. Sugar fermentation test:
Bacteria are grown in a sugar media, and the acid produced is shown with a change in color of the media to red.
b. Litmus milk test:
As the name points out on litmus paper, this test relies on changes in pH.
When bacteria are grown in this medium, there may be the production of acids or alkalis or even no change in pH.
This change is dependent on the type of bacteria.
c. Indole production test
Bacteria are grown in the peptone water culture.
After 48 to 96hrs of incubation at 37°C, it is checked for the presence of red color.
The red color indicates the production of indole from the amino acid tryptophan.
The reagent used is called Kovac’s reagent.
d. Methyl Red test
Bacteria are grown in a glucose phosphate medium at 30°C for five days. Then, a few drops of 0.04% methyl red are added and mixed to observe for color change. The red color indicates a positive, while the yellow color indicates a negative test for glucose-fermenting bacteria.
e. Citrate utilization test
The citrate medium, called Koser’s medium, is used here.
Citrate is the only source of carbon, and its utilization is observed in terms of turbidity.
This test helps identify mostly intestinal gram-negative bacteria.
If positive, it indicates the above-said microbes. See in detail the citrate test.
f. Voges Proskauer Test
Here, to one ml of glucose phosphate medium, 0.6 ml of 5% solution of α-naphthol in ethanol and 0.2 ml of 40% KOH are added.
Acetyl methylcarbinol is produced from pyruvic acid, which is oxidized to diacetyl form to give a red color.
This is a test used to detect bacteria like Enterobacter, Klebsiella. See more details on the VP test.
6. By differential staining
The identification depends on the staining of bacteria.
Most bacteria can be stained by specific stains; for example, Gram +ve bacteria are stained by Gram satin, while Gram -ve bacteria don’t take up Gram stain.
Tuberculous bacteria can be stained by acid-fast stain specifically, and other strains don’t take up this stain.
7. Serological methods.
Here, the identification of bacteria is done by the use of antibodies and antigens, which are specific against the suspected bacteria.
Antigens and antibodies are very specific and bind to a single type of bacteria.
8. By protein and nucleotide analysis.
The cellular constituents like protein content and nucleotide sequence in DNA are used for the identification of bacteria.
This requires methods like Polymerase chain reaction (PCR), gel electrophoresis, radio Immunoassay, etc.
Importance of bacterial Identification
1. Identify the disease
It helps to know the type of infection and the disease caused by the individual.
For example, an acid-fast stain test for Mycobacterium can identify Tuberculosis.
So, bacterial identification is important in health care.
2. Select a suitable drug
Not all drugs (antibiotics) are active against all bacteria.
So, identification helps to target that specific bacteria with a suitable choice of drugs.
For example, rifamycin is best suited for tuberculosis and cannot be controlled by other antibiotics.
3. Evaluation of treatment progress
Identification of bacteria is also necessary to know how far the drug is effective and if the patient is freed from the said bacteria by the treatment.
During the treatment, the patient’s body samples are repeatedly checked during the course to see if there is a recovery in the patient.
This is ascertained by performing an identification test for the causative bacteria. An indication of a negative result in the test indicates he is free from infection.
4. For industrial purposes
It also helps isolate a specific strain of bacteria needed for research or other industrial productions like fermentation etc.
Many vitamins (B12), hormones (insulin), and supplements are produced by rDNA technology by using the principles of biotechnology.
5. For storage
Some bacteria are specifically stored with the intention of future requirements. Identification is also necessary to store the bacteria in pure form without foreign contamination.
These stored bacteria are supplied when required for research or industrial manufacture.
Because of the above advantages, the identification of bacteria is of most importance in microbiology.
Unlike a virus, bacteria are easily traceable by simple staining methods.
Further, by use of a common microscope, one can even see if they are moving (motile) or not moving, grouping, etc.
Identification of bacteria is a part of the diagnosis of many diseases and hence is a good demand for microbiologists.

I’ve been doing some reading about buffered peptone water, and I wanted to do a little more research. I’m glad you talked about how peptone water can grow bacteria. I’m going to have to look into some different buffered peptone water and see what I can find!